Diabetes Can Cause Blindness

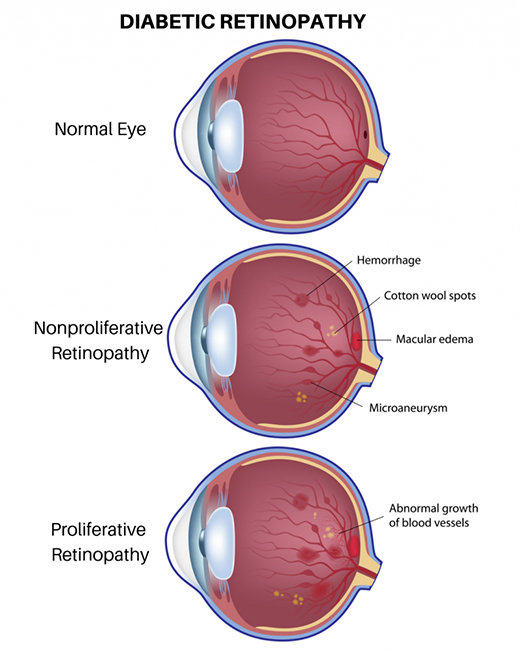 Between 25% and 35% of Australians report some form of diabetic retinopathy.
Between 25% and 35% of Australians report some form of diabetic retinopathy.
Diabetic Retinopathy occurs when changes in blood glucose levels cause changes in retinal blood vessels. In some cases, these vessels will swell up (macular oedema) and leak fluid into the rear of the eye. In other cases, abnormal blood vessels will grow on the surface of the retina and unless treated, diabetic retinopathy can gradually become more serious and progress from ‘background retinopathy’ to seriously affecting vision and can lead to blindness.
I wrote this blog post about a year ago now: ‘5 Tips on How to Prevent Diabetic Eye Disease’. I am now returning to this subject because although we all know that prevention is better than cure, I believe that we live in a curative world, not prophylactic. A lot of us do not want to believe that we might fall victim to one or many diseases. We also mostly believe that if we do; medicine, doctors and surgery can help us with little consequence.
If you have been diagnosed with diabetes or pre-diabetes; you can still help yourself (please refer to my blog post mentioned above about lifestyle choices that will help reduce the rate of progression of diabetic retinopathy). Changing our habits and lifestyle is not easy. Please seek support from family, friends, health professionals and others experiencing the same in a support group setting.

Treatment for diabetic retinopathy
Laser treatment – there are 2 different types of laser treatment available depending on what is required. One is a focal laser treatment called photocoagulation and the other is a scatter laser treatment called panretinal photocoagulation. These treatments are designed to stop or slow the leakage of bleeds from vessels in the eyes and to shrink the abnormally swollen blood vessels by creating small burns.
If vision loss has already occurred from diabetic retinopathy, treatment will rarely restore any lost vision. The primary aim is to stop/slow any further vision loss.
Vitrectomy – Surgery to remove some or all of the vitreous humor from the eye. Vitrectomy comes with a list of possible complications/side effects such as: infections, excess bleeding, high intra-ocular pressure, retinal detachment, lens damage, increased rate of cataract formation and difficulty with eye movement.
Intravitreal Injections – Diabetes is a lifelong condition. You can help to treat the side effects along the way and intravitreal injections is another way of doing this. An Ophthalmologist will carefully inject your eye(s) vitreous (the gel-like fluid that fills the eye) with a medication designed to block the effects of growth signals the body sends to generate new blood vessels. Anti-VEGF (vascular endothelial growth factor) is the name of the medication used and you are required to have these injections every 4 to 12 weeks.
Resources to help you manage your diabetes and support you through this diagnosis
Diabetes Australia is an available resource who can be contacted on their NDSS Helpline 1800 637 700.
Click here to head to the website for Association of Diabetes Care & Education Specialists.
Diabetes WA provide fact sheets that can be easily printed and kept at home.
These resources provide education, support, emotional well-being and up to date information related to diabetes management.
https://insighteye.com.au/3rd-generation-smile-laser-eye-surgery/
At Insight Eye Clinic, we offer a FREE phone suitability assessment. This way, we can rule out any potential reasons that you might not be a suitable candidate for refractive surgery. If you would like to educate yourself on the types of available treatments available, recovery and costs… please visit our blog page which has a plethora of information that is guaranteed to help you on your quest for visual freedom.