Common Cataract Concerns & Questions
Part 2
Welcome to Part 2 of a 3 part series all about cataract surgery.
 What happens during my cataract procedure?
What happens during my cataract procedure?
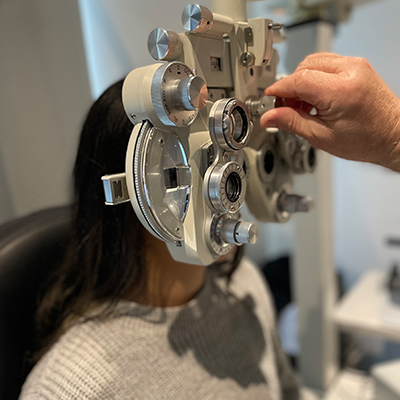
In order to prepare your eye for surgery, your doctor might recommend you begin an antibiotic eye drop 3 days prior to your procedure. On the day of your surgery, your procedure is likely to take only 20 minutes although you will be at the hospital for approximately 3 hours. During this time, you will be met by the nursing staff at Perth Eye Hospital who will go over some pre-admission questions with you and prepare you for your procedure.
Most patients have a local anaesthetic to numb their eyes which is in the form of an eye drop and a mild sedation to help with any nerves or anxiety. Some have a general anaesthetic for various reasons which may include, severe anxiety making them at risk of large movements, underlying health issues, preference and many more. Your eligibility for a GA will be assessed by your anaesthetist.
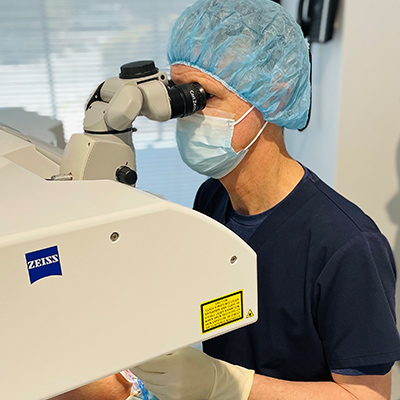
Your doctor will guide you through the procedure and advise you where to focus. You should NOT experience pain during your procedure, occasionally you might experience a small amount of pressure usually preceded with a caution from your doctor. A 2mm slit is made in the cornea and your doctor will use a small instrument to break up and remove the cloudy lens from inside the eye. Once removed, your doctor will then insert the new lens and position it in place. No sutures are needed as the incision is so small and your eye begins to heal immediately.
A quick post-operative check is performed on the day of your procedure or the following morning to check the pressure of the eye as it is very common to see a temporary increase in ocular pressure after surgery. Various solutions are available if you experience this so please do not be alarmed. (Click here for a video overview of cataract surgery)
What visual outcome can I expect from my cataract surgery?
- Monovision (aka blended vision) – Monofocal lenses are used to correct the dominant eye for distance vision and the other for near vision meaning it is unlikely you will require glasses after your procedure but in some cases, people require glasses for finer tasks such as needlework or very small print or long distance night driving. 20% of people’s brains cannot adapt to this visual result and find they experience a sea-sick feeling or problems with depth perception. A contact lens trial is sometimes necessary and allows us to simulate monovision which is how your doctor determines the suitability of this visual outcome. Other procedure types are available for those that cannot adapt to monovision. For the 80% who’s brains’ do agree with this outcome, they are generally extremely happy.
- Trifocal lenses – Trifocal lenses feature a series of rings which diffract light to allow you to have very good distance, intermediate and near vision. The same lens is used in both eyes meaning that you will not experience the same imbalance that some get from monovision. Dr Furness from Insight Eye Clinic has researched the most advanced lenses to give his patients the best possible visual result when having their cataract procedure. Follow this video link for a visual demonstration on how Trifocals could benefit you.
- Distance vision in both eyes – Using a monofocal lens to correct both eyes for distance vision means that you will require reading glasses after your procedure, even if they were not required before. Some people prefer both eyes for distance vision if they experienced an imbalance with monovision, a large amount of glare or halo’s with trifocals or are happy to wear reading glasses. We find that the people who are most happy with this visual outcome, typically have a very high refractive error before their procedure. This visual outcome might also be preferable for occupational reasons. For ex: truck drivers who rely heavily on sharp distance vision without risk of glare or halo’s at night.




Follow Us!